Risks: Suboxone Treatment Addiction?

RRIH Team Member
Date Published: 3/16/2026

Table of Contents
If you or someone you love is considering Suboxone treatment, one of the most common concerns people express is this: “Am I just trading one drug for another?” It’s a fair question, and one that many people ask before they begin treatment for opioid use disorder (OUD) or another substance use disorder (SUD).
The truth is that Suboxone is one of the most effective tools available for treating opioid addiction and has, for decades, been successfully paired with proven behavioral health support to help people achieve stability. When prescribed by an experienced practitioner trained in addiction medicine—such as Dr. Tom Reach at Reach Recovery and Integrated Health, serving patients throughout the Asheville area—and used as part of a comprehensive medication-assisted treatment (MAT) program, Suboxone can reduce cravings, stabilize brain chemistry, and dramatically lower the risk of relapse and overdose. Understanding how this medication works can help separate myth from reality.

In This Article You Will Learn
• Whether Suboxone can actually cause addiction
• The difference between addiction and physical dependence
• How Suboxone works to treat opioid use disorder (OUD)
• How medication-assisted treatment (MAT) and holistic, evidence-based care help people begin and sustain recovery
Is Suboxone Treatment Just Replacing One Drug with Another?
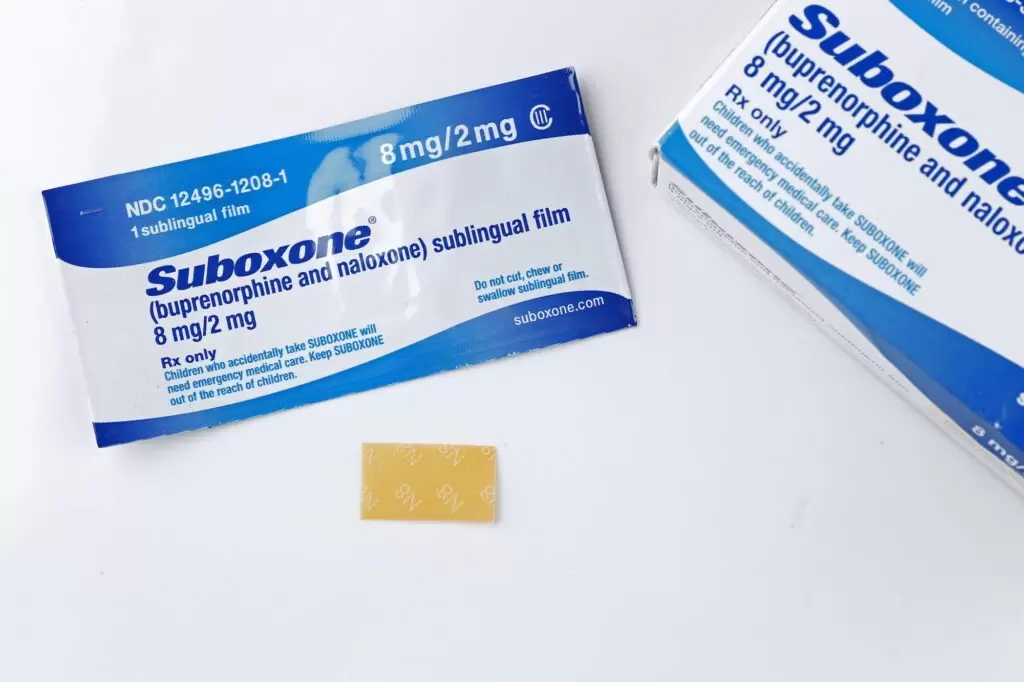
This is one of the most common questions people ask when they first learn about Suboxone treatment. At first glance, the concern may seem reasonable. After all, Suboxone is a medication that interacts with the same opioid receptors in the brain as drugs like heroin, fentanyl, or prescription painkillers.
However, Suboxone is not the same thing as those drugs. Suboxone is a combination medication made up of two components: buprenorphine and naloxone.
Buprenorphine is a partial opioid agonist. It activates opioid receptors in the brain just enough to reduce withdrawal symptoms and cravings, but not enough to produce the intense euphoric effects associated with addictive opioid drugs. This helps stabilize brain chemistry so that patients can focus on recovery rather than constantly battling cravings.
Naloxone is included as a safeguard to discourage misuse. When Suboxone is taken as prescribed sublingually (under the tongue), naloxone is poorly absorbed and has little to no effect. However, if someone attempts to misuse the medication by injecting it, naloxone becomes active and can block opioid effects and trigger withdrawal.
For many patients, working with an experienced Suboxone doctor at a reputable Suboxone clinic provides the structure and medical oversight needed to safely treat opioid use disorder (OUD). When Suboxone treatment is combined with behavioral health support and recovery-focused care, it becomes a powerful tool that helps people move away from the destructive cycle of opioid addiction and toward long-term stability.
Rather than simply replacing one drug with another, medication-assisted treatment (MAT) helps restore balance so that recovery can begin.
What Is the Difference Between Addiction and Physical Dependence?

One of the biggest sources of confusion surrounding Suboxone treatment is the difference between addiction and physical dependence. These two terms are often used interchangeably in everyday conversation, but medically they mean very different things.
Addiction is a pattern of compulsive drug use despite harmful consequences. A person struggling with addiction may continue using drugs even when it damages their health, relationships, employment, or financial stability—and sometimes even when it jeopardizes their freedom through arrests, jail, or prison.
People suffering from addiction still have priorities such as family, work, and relationships. The tragedy of addiction is that those priorities gradually become overshadowed by the overwhelming drive to obtain and use drugs. Over time, the pursuit of the substance can begin to dominate nearly every decision a person makes.
Physical dependence, on the other hand, simply means that the body has adapted to a medication. When someone is physically dependent on a substance, stopping it suddenly can lead to withdrawal symptoms. This can happen with many medications that are used appropriately under medical supervision.
In fact, physical dependence occurs with a wide range of medications, including certain antidepressants, blood pressure medications, and even steroids.
In modern medicine, opioid use disorder (OUD) is understood as a chronic medical condition that affects brain chemistry and behavior. In that sense, it is not unlike other serious health conditions such as diabetes, heart disease, or asthma—conditions that often require ongoing treatment and medication in order for people to live stable and functional lives.
With Suboxone treatment, the goal is not to create a new addiction, but to stabilize the brain so that people suffering from opioid use disorder can focus on recovery. Under the care of a qualified Suboxone doctor at a reputable Suboxone clinic, medication-assisted treatment (MAT) helps patients safely manage withdrawal symptoms, reduce cravings, and rebuild healthy, productive lives.
How Does Suboxone Work to Treat Opioid Use Disorder?

To understand how Suboxone treatment works, it helps to understand what long-term opioid use does to the brain.
Opioids such as heroin, fentanyl, and prescription painkillers attach to specialized sites in the brain known as opioid receptors, which play a role in regulating pain, reward, and breathing. Over time, repeated opioid use disrupts the brain’s normal chemistry. The brain begins to rely on the presence of opioids simply to feel normal.
As opioid use continues, the brain reduces its own production of certain natural chemicals that help regulate pain, stress, and discomfort. One of the systems involved includes a neurotransmitter called norepinephrine, which plays an important role in how the body responds to stress and maintains balance. When opioid use suddenly stops, these natural systems are no longer functioning normally. As a result, people often experience the severe discomfort, anxiety, agitation, and powerful cravings associated with opioid withdrawal.
This is where Suboxone helps.
The medication’s primary ingredient, buprenorphine, is what physicians call a partial opioid agonist. It activates opioid receptors in the brain just enough to reduce withdrawal symptoms and cravings, but not enough to produce the powerful euphoric effects associated with addictive opioid drugs.
Buprenorphine also has what is known as a “ceiling effect.” After a certain dose, taking more of the medication does not significantly increase its opioid effects. This makes Suboxone much safer than full opioid drugs and greatly reduces the risk of misuse or overdose when taken as prescribed.
For patients receiving care from a qualified Suboxone doctor at a reputable Suboxone clinic, this stabilization allows the brain and body to regain balance. Cravings become manageable, withdrawal symptoms are controlled, and patients can begin focusing on rebuilding their lives through recovery-oriented care.
Unfortunately, medication-assisted treatment (MAT) has sometimes been misunderstood, and stigma surrounding addiction treatment still exists in some communities. In many ways, this stigma reflects a broader misunderstanding that has historically surrounded mental and behavioral health care in general. For many years, people seeking help for conditions such as depression, anxiety, and other mental health challenges also faced similar bias. Much of this stigma has been rooted in fear or misunderstanding about how brain chemistry and mental health actually work.
In reality, modern addiction medicine recognizes Suboxone treatment as one of the most effective tools available for helping people recover from opioid use disorder (OUD). By stabilizing brain chemistry and reducing cravings, Suboxone allows patients to think more clearly, regain stability, and focus on the long-term work of recovery.
Where Can You Find Reputable, Evidence-Based Suboxone Treatment in Asheville and Western North Carolina?

For individuals struggling with opioid use disorder (OUD), seeking help can feel overwhelming. Many people delay treatment because they are unsure where to turn, or because they worry about stigma and misunderstanding. The most important step, however, is simply reaching out to a qualified medical professional who understands addiction and the science of recovery.
Modern Suboxone treatment has helped millions of people worldwide stabilize their lives and begin the process of long-term recovery. When this treatment is provided by an experienced physician and supported by behavioral health care, patients are given the tools they need to manage cravings, regain stability, and begin rebuilding relationships, careers, and personal health.
For residents of Asheville and the surrounding communities of Western North Carolina, treatment is available close to home. At Reach Recovery and Integrated Health, Dr. Tom Reach provides compassionate, evidence-based care for individuals seeking help with opioid addiction. The goal of treatment is not simply to manage withdrawal symptoms, but to help patients move toward lasting recovery and a healthier, more stable life.
If you or someone you love is struggling with opioid addiction, help is available. Medication-assisted treatment, including Suboxone, can provide a safe and effective path forward.
To learn more about treatment options or to schedule an appointment, contact Reach Recovery and Integrated Health at 828-575-2070. Taking the first step toward recovery may feel difficult, but it can also be the beginning of lasting change.
Related Articles








